Body
Angular Cheilitis
- Inflammation of the angles of the mouth, characterized by fissures, scaling, erythema and crusting (fig. 1).
- Cause is usually multifactorial, due to a primary infection and/or non-infectious causes, such as mechanical irritation, nutritional deficiency or other dermatologic condition.
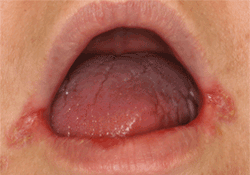 Fig 1. Typical presentation of angular cheilitis with erythema, crusting and mild fissuring of the angles of the mouth bilaterally.
Fig 1. Typical presentation of angular cheilitis with erythema, crusting and mild fissuring of the angles of the mouth bilaterally.
Presentation
Population
- Individuals with increased folding or wrinkling of skin at the corners of the mouth
- Individuals wearing dentures with decreased vertical dimension of occlusion
- Saliva pools in the fissures, creating a chronic moist environment for infection with Candida albicans, Staphylococcus aureus and/or Streptococcus (rare)
- Individuals with underlying systemic conditions including endocrine disorders (e.g., diabetes), immunological disorders (e.g., HIV infection), nutritional deficiencies, hematologic malignancies or solid organ malignancies
Signs
- Red, scaly fissured lesions at the angles of the mouth, usually bilateral
Symptoms
- Pain severity: can range from asymptomatic to severe discomfort
- Burning
- Irritation
- Pruritis
Investigation
- If the patient wears dentures: Are the dentures stable and comfortable? Is the vertical dimension of occlusion appropriate?(Poorly fitting dentures could cause the wrinkling that creates a favorable environment for the condition to manifest.)
- Does the patient have a tendency to lick their lips/corners of mouth?
- Have there been any recent changes to saliva quality or quantity?
- Does the patient report oral burning or taste alterations, which may be indicative of a generalized oral fungal infection? If present, it could be a source of re-infection.
- Ask the patient about any recently prescribed medications (including antibiotics) that may cause this condition.
- Obtain a thorough dental and medical history.
- Recognize responses to review of systems that raise suspicion for underlying systemic disorders.
- Determine the stability of current medical conditions.
- Tobacco use may predispose to the development of this condition.
- If a more thorough investigation is warranted, refer for cytology culture or laboratory assessment to rule out local or systemic predisposing factors.
Diagnosis
Based on clinical finding of erythematous fissures at the angles of the mouth, a diagnosis of angular cheilitis is determined.
Differential Diagnosis
- Contact dermatitis
- Actinic cheilitis
Treatment
Common Initial Treatments
- Initial evaluation of predisposing local factors:
- Evaluation of prostheses
- Maintenance of oral hygiene
- Maintenance of prosthesis hygiene
- Local salivary gland issues
- Intraoral fungal infection
- Prescribe a topical ointment or cream:
- Usually a combination of topical antifungal and antibacterial (e.g., nystatin and mupirocin); consider the use of combination antifungal/antibacterial/glucocorticosteroid ointment (e.g., Viaderm-K.C.® ointment) as an alternative.
- Apply a thin layer to the angles of the mouth 2–3 x daily for 2 weeks.
- Patients should use a new toothbrush when management is started as their toothbrush may be contaminated.
- If an intraoral fungal infection is present, appropriate therapy should be initiated.
Follow Up
Follow up recommended at 2 weeks:
- If the condition is resolved: continue monitoring.
- If the condition is not resolved: consider prescribing an appropriate systemic antifungal.
- If systemic issues are suspected as a cause: the patient should be referred to their primary care physician for additional evaluation and/or management.
THE AUTHORS
Suggested Resources
- Neville BW, Damm DD, Allen CM, Bouquot JE. Erythematous candiasis. In: Oral and Maxillofacial Pathology. 3rd ed. St. Louis: Saunders Elsevier; 2009. p. 214, 216–17.
- Farah CS, Lynch N, McCullough MJ. Oral fungal infections: an update for the general practitioner. Aust Dent J. 2010;55(Suppl 1):48–54.
- Giannini PJ, Shetty KV. Diagnosis and management of oral candidiasis. Otolaryngol Clin N Am. 2011;44(1):231–40.
- Park KK, Brodell RT, Helms SE. Angular cheilitis, part 1: local etiologies. Cutis. 2011;87(6):289–95.
- Park KK, Brodell RT, Helms SE. Angular cheilitis, part 2: nutritional, systemic and drug-related causes and treatment. Cutis. 2011;88(1):27–32.
- Sharon V, Fazel N. Oral candidiasis and angular cheilitis. Dermatol Ther. 2010;23(3):230–42.



