Complications following treatment of mandibular angle fractures are common, and rates as high as 32% have been reported.1-3 Poor patient compliance, medical comorbidities, the complex biomechanical forces that occur at this anatomic location, the presence of wisdom teeth and the difficulty of achieving rigid fixation are among the reasons for this unusually high rate of complications for a fracture.1,2,4-6 Because of all the factors involved, especially poor patient compliance, it is difficult to implement good prospective studies on a reasonable amount of patients, hence, the equivocal data available in the literature.
A recent systematic review and meta-analysis was carried out to identify the best fixation method for these fractures.4 The authors concluded that the use of a single mini-plate (on the external oblique ridge or on the lateral aspect of the mandible) was superior to using a combination of 2 mini-plates to reduce post-operative complications, even though the latter technique has been demonstrated to be biomechanically advantageous. This was confirmed more recently in another study focusing on the best type of fixation.7 However, the heterogeneity of the studies selected for the meta-analysis makes conclusions difficult, and there is still a lack of evidence to support 1 technique over another to treat this type of trauma.
At our institution, there is no standard protocol for treating mandibular angle fractures. The type of fixation chosen is based mainly on surgeons' preference. Extraction of a wisdom tooth that is in the line of fracture, when there is no clear indication for extraction (i.e., fractured tooth, inability to reduce the fracture because of the tooth, presence of a pathology, decay, infection, loose tooth in the fracture line), is also decided at the time of surgery based on preference rather than a defined protocol.8 The goal of our study was to report the complications associated with mandibular angle fractures and identify variables affecting their occurrence.
Materials and Methods
A retrospective case-series design was used. The study population consisted of patients who presented at the Hôpital de l'Enfant-Jésus with a mandibular angle fracture between 1 Jan. 2009 and 1 Sept. 2013. Inclusion criteria were presence of a mandibular angle fracture (defined as a fracture starting at the junction of the ramus and body on the superior aspect of the mandible and extending inferiorly to the region of the angle), follow up of at least 1 month, a complete medical chart (all pertinent data documented) and post-operative radiographs. Patients were excluded if a reconstruction plate was used as the primary method of fixation or if the fracture was the result of a pathological process, such as a tumour. Because of the retrospective nature of this study, it was granted an exemption by our institution's ethics review board.
The following information was collected for each patient: age, sex, tobacco use, type of fixation, the presence and extraction of a wisdom tooth, antibiotic protocol, follow-up duration and complications. An infection was diagnosed if the medical chart documented purulent discharge, an incision and drainage or the prescription of antibiotics. A non-union was identified as mobility at the fracture site requiring revision surgery to place a larger plate. The need for plate removal was considered a complication only if it became infected, fractured or caused discomfort to the patient.
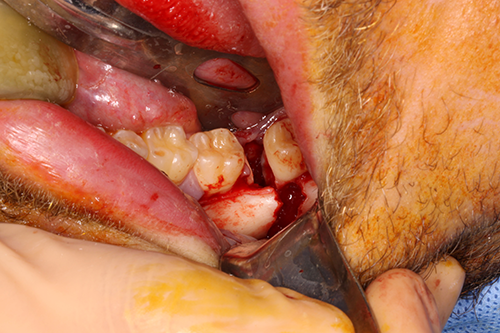
Four types of fixation were used: a sagittal split osteotomy plate (SSOP) (Figs. 1a and 1b), a 2.0-mm plate placed on the lateral border of the mandible, a Champy plate (a 1.5-mm mini-plate along the external oblique ridge) or 2 mini-plates on the lateral border of the mandible. All patients were under general anesthesia during surgery. The fractures were exposed through an intraoral incision along the external oblique ridge; there was no transcervical approach. Patients were then placed in intermaxillary fixation (IMF) with the use of arch bars or intraosseous screws. The fracture was reduced and fixated with one of the 4 techniques. A transbuccal trocar was used when necessary. Guiding elastics were maintained for 0–4 weeks. No rigid postoperative IMF was kept in place. Patients followed a soft diet for 4 weeks and all received a prescription for chlorhexidine gluconate 0.12% oral rinse, twice daily for 7 days.

Figure 1a: Pre-operative left mandibular angle fracture.

Figure 1b: Fixation of the fracture with a sagittal split osteotomy plate.
Every patient received antibiotic prophylaxis consisting of 2 g of intravenous cephazolin (900 mg of IV clindamycin when allergic to penicillin) 30 minutes before the start of the operation and then every 3 h intraoperatively. Some patients received a 7-day prescription of oral antibiotics before discharge from the hospital. The decision to prescribe antibiotics after surgery was based on surgeons' preference. All patients were seen 7–14 days after surgery and 4–6 weeks later. More follow-up visits were scheduled when necessary (e.g., when there were complications).
We used univariate analysis to report frequency data for qualitative variables and means and standard deviations (SD) for quantitative variables. Fisher exact tests, χ2 tests and Student t tests were used to measure the bivariate association between complications and the relevant variables. Multivariate analyses were performed using logistic regression. Statistical significance was defined as p < 0.05 for all tests. All statistical analyses were carried out using SAS software, version 9.3.
Results
Of the 129 patients treated for a mandibular angle fracture during the study period, 78 (73 men) met the inclusion criteria. Ages ranged from 15 to 59 years (mean 25.2 years, SD 9.07). Forty-one patients (52.6%) were smokers. The mean follow-up period was 7.7 months (range 1–38 months, SD 8.15). A wisdom tooth was present in 67 cases (85.9%) and it was removed 62.7% of the time (42 patients). Thirty-four patients (43.6%) had other mandibular fractures: 27 parasymphysis, 5 body and 2 a combination of subcondylar and parasymphysis. All patients received intraoperative antibiotic prophylaxis, but only 26 (33.3%) left with an antibiotic prescription. Most fractures were fixated using an SSOP plate (n = 32; 41.0%) or a 2.0-mm plate on the lateral aspect of the mandible (n = 20; 25.6%). For 16 patients (20.5%), a Champy plate was installed, and for 10 (12.8%) 2 mini-plates were used. The overall complication rate was 42.3% (n = 33); 37.2% infection, 26.9% plate removal and 6.4% non-union. Some patients had a combination of the above mentioned complications. Descriptive statistics are presented in Table 1.
| Variable | No. (%), except where noted* |
|---|---|
| *Continuous measures are mean ± SD (range). Note: SD = standard deviation, SSOP = sagittal split osteotomy plate. |
|
| Sex | |
| Male | 73 (93.6) |
| Female | 5 (6.4) |
| Age, years ± SD (range) | 25.2 ± 9.07 (15–59) |
| Smokers | 41 (52.6) |
| Follow-up, months ± SD (range) | 7.7 ± 8.15 (1–38) |
| Antibiotics | |
| > 24 h | 26 (33.3) |
| ≤ 24 h | 52 (66.7) |
| Other mandibular fractures | 34 (43.6) |
| Wisdom teeth | |
| Extracted | 42 (53.8) |
| Left in place | 25 (32.1) |
| Absent | 11 (14.1) |
| Type of fixation | |
| SSOP plate | 32 (41.0) |
| 2.0-mm plate | 20 (25.6) |
| Champy plate | 16 (20.5) |
| 2 plates | 10 (12.8) |
| Complications | |
| Infections | 29 (37.2) |
| Plates removed | 21 (26.9) |
| Nonunion | 5 (6.4) |
| All complications | 33 (42.3) |
Because the age of the patients did not follow a normal distribution, patients were separated into 2 groups: those above and below the median. Older patients (> 23 years) had more infections (p = 0.03), more plates removed (p = 0.027) and more complications (p = 0.03) (s 2, 3 and 4). Plates had to be removed more frequently in smokers (p < 0.05). The only other variable that was significantly associated with increased complications was the extraction of a wisdom tooth. When a wisdom tooth was extracted, more infections (p = 0.04) and more overall complications (p = 0.02) were observed (Tables 2, 3 and 4).
A logistic regression model confirmed that younger patients (< 23 years) had fewer infections (odds ratio [OR] 0.29, 95% confidence interval [CI] 0.10–0.87, p = 0.03). Similarly, extracting a wisdom tooth had a deleterious effect on wound infections (OR 6.22, 95% CI 1.16–33.48, p = 0.007). Leaving a wisdom tooth in place may also lead to more infections, but this was not significant (OR 1.60, 95% CI 0.25–10.07, p = 0.51) (Table 5).
| Variable | Infection, no. (%) | p | |
|---|---|---|---|
| Yes | No | ||
| Note: SSOP = sagittal split osteotomy plate. | |||
| Sample size | 29 (37.2) | 49 (62.8) | |
| Age | |||
| < 23 years | 11 (37.9) | 31 (63.3) | |
| ≥ 23 years | 18 (62.1) | 18 (36.7) | 0.030 |
| Smokers | 18 (62.1) | 23 (46.2) | 0.196 |
| Other mandibular fractures | 11 (37.9) | 23 (46.9) | 0.438 |
| Antibiotics | |||
| > 24 h | 10 (34.5) | 16 (32.7) | |
| ≤ 24 h | 19 (65.5) | 33 (67.3) | 0.868 |
| Wisdom teeth | |||
| Extracted | 21 (72.4) | 21 (42.9) | |
| Left in place | 5 (17.2) | 20 (40.8) | |
| Absent | 3 (10.3) | 8 (16.3) | 0.040 |
| Type of fixation | |||
| SSOP plate | 13 (44.8) | 19 (38.8) | |
| 2.0-mm plate | 10 (34.5) | 10 (20.4) | |
| Champy plate | 4 (13.8) | 12 (24.5) | |
| 2 plates | 2 (6.9) | 8 (16.3) | 0.323 |
| Variable | Plate removed, no. (%) | p | |
|---|---|---|---|
| Yes | No | ||
| Note: SSOP = sagittal split osteotomy plate. | |||
| Sample size | 21 (26.9) | 57 (73.1) | n/a |
| Age | |||
| < 23 years | 7 (33.3) | 35 (61.4) | |
| ≥ 23 years | 14 (66.7) | 22 (73.1) | 0.027 |
| Smokers | 15 (71.4) | 26 (45.6) | 0.043 |
| Other mandibular fractures | 7 (33.3) | 27 (47.4) | 0.268 |
| Antibiotics | |||
| > 24 h | 10 (47.6) | 16 (28.1) | |
| ≤ 24 h | 11 (52.4) | 41 (71.9) | 0.104 |
| Wisdom teeth | |||
| Extracted | 15 (71.4) | 27 (47.4) | |
| Left in place | 5 (23.8) | 20 (35.1) | |
| Absent | 1 (4.8) | 10 (17.5) | 0.145 |
| Type of fixation | |||
| SSOP plate | 11 (52.4) | 21 (36.8) | |
| 2.0-mm plate | 6 (28.6) | 14 (24.6) | |
| Champy plate | 3 (14.3) | 13 (22.8) | |
| 2 plates | 1 (4.8) | 9 (15.8) | 0.454 |
| Variable | Complications, no. (%) | p | |
|---|---|---|---|
| Yes | No | ||
| Note: SSOP = sagittal split osteotomy plate. | |||
| Sample size | 33 (42.3) | 45 (57.7) | |
| Age | |||
| < 23 years | 13 (39.4) | 29 (64.4) | |
| ≥ 23 years | 20 (60.6) | 16 (35.6) | 0.028 |
| Smokers | 21 (63.6) | 20 (44.4) | 0.094 |
| Other mandibular fractures | 11 (33.3) | 23 (51.1) | 0.118 |
| Antibiotics | |||
| > 24 h | 13 (39.4) | 13 (28.9) | |
| ≤ 24 h | 20 (60.6) | 32 (71.1) | 0.331 |
| Wisdom teeth | |||
| Extracted | 24 (72.7) | 18 (40.0) | |
| Left in place | 6 (18.2) | 19 (42.2) | |
| Absent | 3 (9.1) | 8 (17.8) | 0.017 |
| Type of fixation | |||
| SSOP plate | 15 (45.5) | 17 (37.8) | |
| 2.0-mm plate | 11 (33.3) | 9 (20.0) | |
| Champy plate | 4 (12.1) | 12 (26.7) | |
| 2 plates | 3 (9.1) | 7 (15.6) | 0.249 |
| Variable | Odds ratio (95% CI) | p |
|---|---|---|
| Note: CI = confidence interval. | ||
| Wisdom teeth | ||
| Absent | 1.00 | |
| Extracted | 6.22 (1.16–33.48) | 0.007 |
| Not extracted | 1.60 (0.25–10.07) | 0.509 |
| Age | ||
| ≥ 23 years | 1.00 | |
| < 23 years | 0.29 (0.10–0.87) | 0.028 |
Discussion
In this study, 43% of patients had complications associated with treatment for a mandibular angle fracture, mainly infections (37.2%). In comparison, Ellis and colleagues observed a 19% rate of infection in a cohort of 402 patients.2 de Amaratunga reported a 16.1% infection rate when a tooth in the line of fracture was retained and 13.7% when it was removed.5 The overall rate of infection in Malanchuk and Kopchak's study was 24.7%.6 In a 10-year retrospective study of 322 patients, 28.53% had complications.9 The high rate of infection in our study may be because many patients had to be excluded from our cohort because they did not attend their follow-up appointment, and it is likely that those missing appointments healed well.
The effect of management of a wisdom tooth in the line of fracture on healing and postoperative complications remains controversial, and many studies have shown conflicting results.5,6,8,10-14 In our study, a tooth was present in 67 cases (85.9%), and it was extracted most of the time (in 42 of the 67 cases or 62.7%). As many others have reported, when a tooth was absent, fewer complications were seen; however, we had few patients in this situation (n = 11). When a tooth was present but not extracted, the rate of infection was higher, but not significantly higher (OR 1.60, p = 0.51) than when no tooth was present. However, removal of the tooth resulted in a significantly higher rate of complications (OR 6.22, p = 0.007). This may be explained by a reduction in bony contact in the area of the fracture if bone had to be removed to extract the tooth. Also, if the tooth is partly erupted, primary closure may be more difficult, potentially increasing the risk of wound dehiscence and complications.
Although de Amaratunga found no significant difference in infection rate with or without tooth removal, all patients in that study received postoperative antibiotics for 14 days.5 Ellis and colleagues had similar results, although they do not report the use of postoperative antibiotics.2 In addition to the usual absolute indications to remove teeth in the line of fracture, Ellis and colleagues extracted a tooth if the apical half or more was exposed. This was done to avoid the need for selective extraction later in a population with low socioeconomic status and, presumably, difficulty in accessing dental care. Although this is a logical treatment strategy, if it increases the likelihood of infection at the fracture site, as demonstrated in our study, it may also increase the risk of more serious complications, such as osteomyelitis and non-union.
We opted to treat most fractures with an SSOP plate on the lateral aspect of the mandible, placed with transbuccal instrumentation.15 This type of plate was originally designed for sagittal split osteotomies. It is different from the 3-dimensional strut plate described in other studies, but acts similarly by creating a broad platform with screws at different levels on each side of the fracture.16 A possible benefit of this technique is to reduce rotation of bony fragments along the long axis of the plate.15-19 A meta-analysis showed that a similar technique of fixation (geometric mini-plate) was superior to conventional mini-plates, with a 71% reduction in overall complications.4 Although we did not demonstrate this finding, the number of patients in our study was significantly smaller. The superiority of a single mini-plate over 2 mini-plates to reduce postoperative complications has also been shown, even if the latter technique is biomechanically superior.7 Thus, the technique used to fix these fractures is only 1 of many factors involved in the occurrence of complications.
Many patients (43.6%) in this study had more than 1 mandibular fracture, and this may have affected our results, as a combination of fractures has been reported to affect the biomechanics acting across fractures. In the presence of 2 mandibular fractures, treating at least 1 rigidly has been suggested to decrease complications.20 Of the 34 patients with other fractures treated in this study, rigid fixation of the other fractures, usually the parasymphysis (n = 27), was carried out for all but 2. These 2 patients had a greenstick fracture of the parasymphysis that was explored, but not plated, because of lack of mobility. All subcondylar fractures were treated with open reduction and internal fixation.
Because of the retrospective design of this study, clear criteria for complications were not defined and we had to rely on clinical notes for data collection; this may have affected our results. However, when complications were present, action had to be taken (prescription of antibiotics, incision and drainage, further fixation) and this information was easily found in medical charts, thus reducing the risk of underestimation. Another weakness of this study is its limited number of patients. We had to exclude 51 patients from our cohort, mainly because of insufficient follow-up time. However, our strict inclusion criteria and extended follow-up period (mean 7.7 months) increases the reliability of our results.
Conclusion
Open reduction with internal fixation of mandibular angle fractures is associated with a high rate of complications. The extraction of a wisdom tooth in the line of fracture may increase the risk of complications.
THE AUTHORS
The authors have no declared financial interests.
This article has been peer reviewed.
References
- Patel N, Kim B, Zaid W. A detailed analysis of mandibular angle fractures: epidemiology, patterns, treatments, and outcomes. J Oral Maxillofac Surg. 2016;74(9):1792-9.
- Ellis E 3rd. Outcomes of patients with teeth in the line of mandibular angle fractures treated with stable internal fixation. J Oral Maxillofac Surg. 2002;60(8):863-5.
- Gear AJ, Apasova E, Schmitz JP, Schubert W. Treatment modalities for mandibular angle fractures. J Oral Maxillofac Surg. 2005;63(5):655-63.
- Al-Moraissi EA, Ellis E 3rd. What method for management of unilateral mandibular angle fractures has the lowest rate of postoperative complications? A systematic review and meta-analysis. J Oral Maxillofac Surg. 2014;72(11):2197-211.
- de Amaratunga NA. The effect of teeth in the line of mandibular fractures on healing. J Oral Maxillofac Surg. 1987;45(4):312-4.
- Malanchuk VO, Kopchak AV. Risk factors for development of infection in patients with mandibular fractures located in the tooth-bearing area. J Craniomaxillofac Surg. 2007;35(1):57-62.
- Al-Moraissi EA. One miniplate compared with two in the fixation of isolated fractures of the mandibular angle. Br J Oral Maxillofac Surg. 2015;53(8):690-8.
- Shetty V, Freymiller E. Teeth in the line of fracture: a review. J Oral Maxillofac Surg. 1989;47(12):1303-6.
- Seemann R, Schicho K, Wutzl A, Koinig G, Poeschl WP, Krennmair G, et al. Complication rates in the operative treatment of mandibular angle fractures: a 10-year retrospective. J Oral Maxillofac Surg. 2010;68(3):647-50.
- Kahnberg KE, Ridell A. Prognosis of teeth involved in the line of mandibular fractures. Int J Oral Surg. 1979;8(3):163-72.
- Neal DC, Wagner WF, Alpert B. Morbidity associated with teeth in the line of mandibular fractures. J Oral Surg. 1978;36(11):859-62.
- Ramakrishnan J, Shingleton A, Reeves D, Key JM, Vural E. The effects of molar tooth involvement in mandibular angle fractures treated with rigid fixation. Otolaryngol Head Neck Surg. 2009;140(6):845-8.
- Thaller SR, Mabourakh S. Teeth located in the line of mandibular fracture. J Craniofac Surg. 1994;5(1):16-9.
- Zanakis S, Tasoulas J, Angelidis I, Dendrinos C. Tooth in the line of angle fractures: the impact in the healing process. A retrospective study of 112 patients. J Craniomaxillofac Surg. 2015;43(1):113-6.
- Braasch DC, Abubaker AO. Management of mandibular angle fracture. Oral Maxillofac Surg Clin North Am. 2013;25(4):591-600.
- Al-Moraissi EÀ, El-Sharkawy TM, El-Ghareeb TI, Chrcanovic BR. Three-dimensional versus standard miniplate fixation in the management of mandibular angle fractures: a systematic review and meta-analysis. Int J Oral Maxillofac Surg. 2014;43(6):708-16.
- Guimond C, Johnson JV, Marchena JM. Fixation of mandibular angle fractures with a 2.0-mm 3-dimensional curved angle strut plate. J Oral Maxillofac Surg. 2005;63(2):209-14.
- Vineeth K, Lalitha RM, Prasad K, Ranganath K, Shwetha V, Singh J. "A comparative evaluation between single noncompression titanium miniplate and three dimensional titanium miniplate in treatment of mandibular angle fracture" — a randomized prospective study. J Craniomaxillofac Surg. 2013;41(2):103-9.
- Kalfarentzos EF, Deligianni D, Mitros G, Tyllianakis M. Biomechanical evaluation of plating techniques for fixing mandibular angle fractures: the introduction of a new 3D plate approach. Oral Maxillofac Surg. 2009;13(3):139-44.
- Ellis E 3rd. Open reduction and internal fixation of combined angle and body/symphysis fractures of the mandible: how much fixation is enough? J Oral Maxillofac Surg. 2013;71(4):726-33.