Body
Recurrent Herpes Simplex
- Primary and recurrent infection with herpes simplex virus (HSV-1 and HSV-2) can cause oral and/or genital lesions, although the majority of oral infections are caused by HSV-1.
- Primary HSV infection can manifest with clinical symptoms of fever, sore throat, lymphadenopathy and general malaise, although many infections are subclinical.
- Symptomatic vesicles/ulcers of the oral mucosal tissues generally follow the onset of systemic symptoms and are often accompanied by significant erythema of the gingival tissues (i.e., primary herpetic gingivostomatitis).
- Treatment of primary HSV infections is usually palliative, while the majority of infections resolve within 2 weeks of symptom onset.
- HSV can establish latency in the trigeminal ganglia and may periodically reactivate.
Transmission of HSV may occur at a low rate via salivary transfer in the absence of observable lesions.
Presentation
Population
- Recurrent herpes simplex labialis (HSL)
- More commonly seen in healthy individuals.
- Presents across the age spectrum, from adolescents to the elderly.
- Common triggers include UV light, physical/emotional stress, upper respiratory tract illness, cold weather, hormonal changes, and mouth/lip trauma.
- Recurrent intraoral herpes (RIH)
- More commonly seen in immunocompromised individuals.
Signs
- Recurrent HSL
(Fig. 1)- Presents as fever blisters or cold sores.
- Lesions at the mucocutaneous junction of the lips.
- Begin as vesicles that rupture, leaving superficial ulcers that crust and heal—usually without scarring—within 2 weeks.
- RIH
(Fig. 2)- Crop(s) of vesicles that often rupture and leave ulcers on keratinized and/or non-keratinized oral mucosa.
- When RIH occurs in immunocompetent hosts, involvement is typically limited to the keratinized tissue, especially the hard palate, and is almost always unilateral.
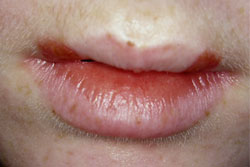 Figure 1. Bilateral recurrent herpes labialis lesions.
Figure 1. Bilateral recurrent herpes labialis lesions.
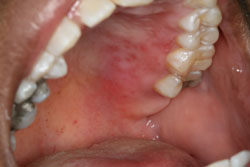 Figure 2. Recurrent intraoral herpes lesions affecting the palate.
Figure 2. Recurrent intraoral herpes lesions affecting the palate.
Symptoms
- Pain severity can range from asymptomatic to severe.
- HSL is often preceded by prodrome involving tingling, itching, and/or burning.
Investigation
Rule Out Local Pathology
- Obtain patient history. If patient reports history of primary herpetic gingivostomatitis and/or recurrent HSL, note:
- Location of lesions
- Frequency and duration of lesions
- Symptoms associated with lesions
- Known triggers for development of lesions
- Post-disease course and/or complications associated with lesions
- Overall medical history, especially for patients with suspected RIH
- Investigation
- Diagnosis is primarily based on clinical findings considering history, location, and appearance of lesions. Further investigation is generally not warranted.
- For patients with atypical lesions or with suspected RIH, cytology evaluation, biopsy, and PCR assessment may be considered. Patients should be referred to the appropriate dental or medical specialist for such tests to be conducted.
Diagnosis
- Diagnosis of RHL is primarily based on history and clinical examination. Atypical RHL lesions and/or RIH may require further investigation and patients should be referred to dental and/or medical providers with expertise in this area.
Differential Diagnosis
- Typical recurrent HSL lesions are generally pathognomonic for this condition.
- RIH may appear similar to traumatic lesions (mechanical/thermal/chemical) or other types of oral mucosal disorders, such as aphthous stomatitis.
Treatment
Common Initial Treatments
- Patient education regarding the nature of the condition:
- Contagious nature of disease: limit personal contact while lesion is active, especially transfer of saliva
- Importance of meticulous hygiene
- Exploration of triggers for lesion development:
- Prophylactic treatment may be considered for patients if they are exposed to known triggers
- Symptomatic relief:
- Ice application
- Lanolin application
- Topical antiviral application may be considered based on frequency and severity of lesions:
- Penciclovir 1% (e.g., Denavir ®) (if available): by prescription only, apply to lesion every 2 hours from the time of the prodrome until the lesion has healed.
- Acyclovir 5%: apply to lesion every 2 hours from the time of the prodrome until the lesion has healed.
- Docosanol 10% (e.g., Abreva ®): apply to lesion every 2 hours from the time of the prodrome until the lesion has healed.
Intervention
- Possible interventions based on frequency and severity of lesions:
- Abortive Therapy: Valacyclovir 2000 mg twice a day for one day or famciclovir 500 mg 2-3 times a day when the patient experiences prodromal symptoms.
- Active Therapy: Acyclovir 400 mg 3 times a day for 5 to 7 days.
- Prophylaxis Therapy: Sunscreen alone (SPF 15 or higher) or acyclovir 400 mg 2-3 times a day or valacyclovir 500 to 2000 mg twice a day.
- Suppressive Therapy: This may be considered for patients with frequent, severe, and disfiguring RHL episodes. Patients should be referred to the appropriate dental or medical specialist for this type of management.
- RIH: Immunocompromised patients with this condition may require extended courses of systemic antivirals and should be referred to the appropriate dental or medical specialist for this type of management.
Follow Up
- Active lesions: 2 weeks
- No active lesions but known history of recurrent HSL: in conjunction with routine dental care
Advice
- It is unusual for lesions to not respond to typical antiviral agents. However, some lesions may be resistant to typical medications.
- If lesion does not resolve with application of usual medications, further investigation is warranted.
- Elective dental treatment should be deferred for patients with active lesions as aerosolization of the virus may occur during dental procedures, placing both the patient and oral health care provider at risk for possible infection or re-infection.
THE AUTHORS
Suggested Resources:
- Stoopler ET. Oral herpetic infections (HSV 1–8). Dent Clin North Am. 2005; 49(1):15–29.
- Stoopler ET, Pinto A, DeRossi SS, Sollecito TP. Herpes simplex and varicella-zoster infections: clinical and laboratory diagnosis. Gen Dent. 2003;51(3):281-6; quiz 287.
- Balfour HH Jr. Antiviral drugs. N Engl J Med. 1999;340(16):1255-68.
- Fatahzadeh M, Schwartz RA. Human herpes simplex virus infections: epidemiology, pathogenesis, symptomatology, diagnosis, and management. J Am Acad Dermatol. 2007;57(5):737-63; quiz 764-6.
- Arduino PG, Porter SR. Oral and perioral herpes simplex virus type 1 (HSV-1) infection: review of its management. Oral Dis. 2006;12(3):254-70.
- Cunningham A, Griffiths P, Leone P, Mindel A, Patel R, Stanberry L, Whitley R. Current management and recommendations for access to antiviral therapy of herpes labialis. J Clin Virol. 2012; 53(1):6-11.
- Fatazadeh M, Schwartz RA. Human herpes simplex labialis. Clin Exp Dermatol. 2007;32(6):625–30.
- Woo SB, Challacombe SJ. Management of recurrent oral herpes simplex infections. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103 Suppl: S12.e1-18.



