Abstract
Correlations with periodontitis have been reported for several diseases, although the biological mechanisms that might lead to these putative correlations are generally unclear. This paper describes the most robust of these associations, on the basis of an evaluation of research syntheses (meta-analyses and systematic reviews) available up to June 2011. This high-level evidence indicates that individuals with periodontitis have a significantly higher risk of various other problems, including cardiovascular disease, diabetes mellitus, respiratory disease and preterm low-birth-weight deliveries. For some conditions, treatment of periodontitis leads to a reduction in the rates of the other disease, lending further support to the concept that the association is reversible. An understanding of these correlations is important to allow dental health care providers to inform patients with periodontitis of their increased risks and to counsel such patients to seek additional medical assessment or intervention, as indicated.
Introduction
Since publication of the US Surgeon General’s report on oral health in the year 2000,1 there has been increased interest in determining whether a link exists between oral health and overall health or disease. Several diseases appear to be correlated with periodontitis, but the mechanisms are generally unknown. Despite the biological plausibility of some of these associations, the biggest challenge is sifting through and analyzing the published evidence to determine which are robust and which are only tenuous or weak. An understanding of the strength of the proposed associations is important so that patients with periodontitis can be informed of the risks (especially if they have other risk factors for an associated condition or disease) and can be counselled to seek further medical assessment. Such assessment may be considered prophylactic or may be related to the medical management of the particular disease or diseases for which the patient has an elevated risk.
To establish as firmly as possible the association between certain health conditions and periodontal diseases, the literature was searched to identify the strongest of these associations, as indicated in formal research syntheses available to February 2012. Such formal research syntheses allow decision-making on the basis of the best available evidence, both quantitative (meta-analyses) and qualitative (systematic reviews). These evidence-based decisions have greater power and precision, with less bias, than decisions based on the results of any single study.
More specifically, an individualized search strategy was defined in Ovid MEDLINE to identify meta-analyses for each systemic disease category. Keywords were auto-exploded to the Medical Subject Heading (MeSH) terms “periodontal diseases” and the related terms for each systemic disease category: “cardiovascular diseases,” “diabetes mellitus,” “pregnancy outcomes,” “preeclampsia” and “respiratory disorders.” The search was limited to English-language articles (meta-analyses and systematic reviews). After screening of titles and abstracts, 15 papers were retrieved and examined in further detail to serve as the evidence for this study. Where a significant association between periodontal disease and another systemic condition was demonstrated, we evaluated the “reversibility” of the associated condition by determining whether periodontal treatment was followed by a reduction in the rates of the related disease or risks for the disease. It is important to note that demonstration of such reversibility may be affected by known or unknown confounders.2 Nonetheless, reversibility of a related condition with periodontal treatment lends additional credibility to the proposed association.
The diseases for which an association with periodontitis has been reported include cardiovascular disease (CVD), stroke, respiratory disease, rheumatoid arthritis, pancreatic cancer, diabetes mellitus (types 1 and 2), preterm delivery, low-birth-weight delivery, preeclampsia, osteoporosis and osteoarthritis. On the basis of an initial scan of the literature for high-level evidence, data were analyzed for only a selection of these conditions: CVD, diabetes, adverse outcomes of pregnancy, preeclampsia and respiratory disease.
Cardiovascular Disease
CVD has always been one of the leading causes of death in Canada. For example, in 2004, there were 72 743 deaths due to CVD, representing 32.1% of all deaths. In 2000, CVD costs in Canada amounted to $22.2 billion. Direct costs (e.g., for hospital care, prescription drugs and physician care) accounted for $7.6 billion, and $14.6 billion was attributed to economic output lost due to disability or death in 2000.3
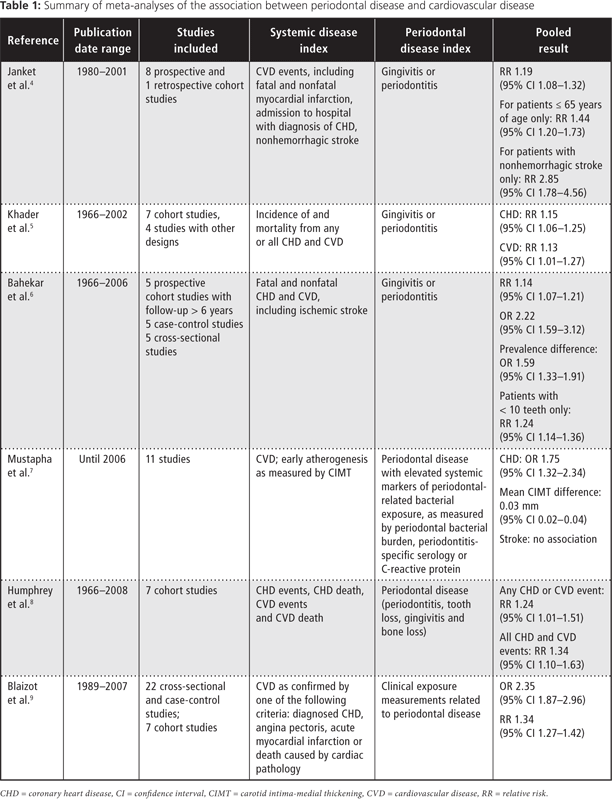
Six meta-analyses4-9 published between 2003 and 2009 showed a weak but statistically significant association between CVD and periodontal disease (Table 1). Although the risk estimates (generally relative risk and/or odds ratio [OR] less than 2) might be considered modest, the high prevalence of both types of disease means that the absolute numbers of those affected is quite high. Hence, on the basis of these meta-analyses, it can be concluded that an individual with periodontitis is at greater risk of either having or developing CVD.
A pathophysiological link may exist between periodontitis and CVD, although it would be difficult to demonstrate. A meta-analysis of studies conducted between 1966 and 2005 concluded that periodontal treatment had no effect on serum levels of C-reactive protein (CRP; a surrogate risk marker for CVD) at 2 months after the treatment.10 The same conclusion was reached from analysis of pooled data from single cohort studies (mean overall difference in CRP 0.2 mg/L, 95% confidence interval [CI] –0.15 to 0.55 mg/L; p > 0.05). Therefore, it appears that periodontal therapy has no consistent effect on CRP levels, which could lead to the conclusion that CVD would not be reversed by periodontal treatment. However, a more recent randomized controlled trial11 compared the effects of intensive treatment of periodontitis (including extractions) with the effects of supragingival scaling and prophylaxis (the latter treatment being ineffective for periodontitis) on endothelial cell function. In that study, the investigators assessed flow-mediated vasodilatation of the brachial artery, because reduced vasodilatation is a surrogate marker for CVD. They also assessed markers of inflammation, coagulation and endothelial activation. Participants who received intensive treatment for periodontitis experienced significantly improved flow-mediated dilatation 60 and 180 days after therapy, whereas those who underwent supragingival scaling had no improvements. There were no between-group differences in serum levels of CRP, which is consistent with data from other studies. These findings indicate that CVD may indeed be reversed by periodontal treatment, further supporting the link between periodontitis and CVD.
Diabetes Mellitus
Diabetes mellitus is characterized by high levels of blood glucose resulting from defects in insulin production, insulin activity or both. There are 2 major forms of this disease.12 Type 1 diabetes (accounting for 5%–10% of cases) is an autoimmune disease that targets pancreatic beta cells; it affects children and young adults. Type 2 diabetes (accounting for 90%–95% of cases) is increasingly being diagnosed in children and adolescents. It begins as insulin resistance, a disorder in which cells lose their ability to respond properly to insulin. As the need for insulin rises, the pancreas gradually loses its ability to produce any insulin at all. Other minor forms of diabetes mellitus, including gestational diabetes, represent only about 1%–5% of cases.
Diabetes is a high-impact disease. In a 2006 meta-analysis,13 the association between both type 1 and type 2 diabetes and periodontal disease was assessed by comparing the extent and severity of periodontal diseases in people with and without diabetes. The evidence (from studies published between 1970 and 2003) consisted of 18 comparative cross-sectional studies, 3 prospective cohort studies and baseline data from 2 clinical trials examining oral hygiene, as well as gingival and periodontal status. People with diabetes had significantly worse oral hygiene (according to plaque index scores; difference 0.218, 95% CI 0.098–0.337) and more severe gingival disease (as measured by average gingival index; difference 0.147, 95% CI 0.012–0.281), as well as more severe periodontitis (according to average probing pocket depth; difference 0.346 mm, 95% CI 0.194–0.498) and clinical attachment loss (difference 0.612 mm, 95% CI 0.462–0.761).
This meta-analysis13 provided evidence to support an association between diabetes and periodontal disease. A Cochrane systematic review14 reported on the reversible relationship (i.e., improvement in glycemic control with periodontal therapy), as indicated by measurements of hemoglobin A1c (HbA1c), an important marker of glucose metabolism. Seven studies were included in the review, 3 of which were also subjected to meta-analysis. The evidence suggested that among people with type 2 diabetes mellitus, periodontal treatment (i.e., scaling, root planing and oral hygiene instructions, with or without antibiotic therapy) led to a mean reduction in HbA1c of 0.4% (95% CI –0.78% to –0.01%) after 3–4 months, relative to no treatment. Although the reduction in mean HbA1c may appear modest at first glance, reductions of only 0.8% in this marker can lead to reductions in end-stage microvascular complications of about 70%;15 as such, even a reduction of 0.4% is important. Nonetheless, further study is needed, and an investigation is now underway.16 Findings showing reversibility with periodontal treatment support results showing statistically significant associations between periodontitis and diabetes, particularly type 2 diabetes.
Adverse Outcomes of Pregnancy
Preterm delivery, an important cause of perinatal mortality and morbidity, is defined as delivery before 37 completed weeks of gestation.17 The frequency of preterm birth in the United States increased from 10.7% in 1992 to 12.3% in 2003.18 In 2009–2010, the Canadian in-hospital preterm birth rate was 8.0%.19 This problem has major social and economic consequences worldwide.18,20 In 2005–2006 in Canada, the average in-hospital cost associated with preterm babies was 9 times higher than for full-term babies among singletons ($9233 vs. $1050) and about 7 times higher among multiple-birth babies ($12 479 vs. $1871).21
Vergnes and Sixou20 performed a meta-analysis to assess the effect of maternal periodontal disease on preterm delivery and/or delivery of infants with low birth weight. The 17 studies (published up to 2005) included in their analysis involved a total of 7151 women, 1056 of whom delivered a preterm and/or low-birth-weight infant. The chance of a preterm birth was about 3 times higher among mothers with periodontitis, relative to healthy participants who did not have periodontitis (OR 2.83, 95% CI 1.95–4.10, p < 0.0001), which indicates an association between periodontitis and this adverse outcome. However, the authors cautioned that among the included studies, those that were more carefully designed demonstrated a weaker association. The authors also concluded that pooled values should be interpreted with caution until the results are confirmed in larger, well-designed multicentre trials.
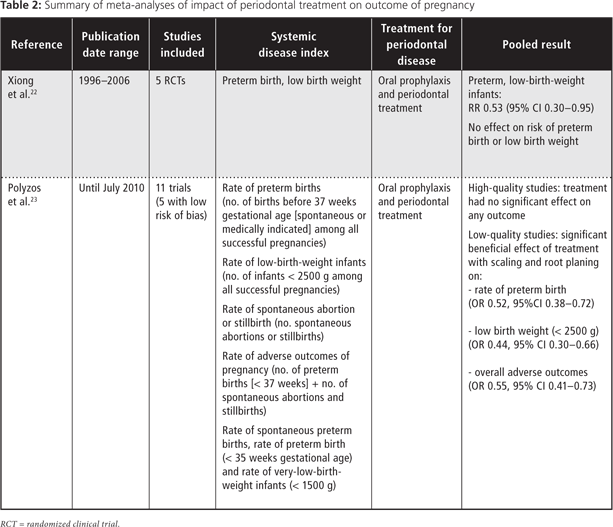
Taken together, the available evidence supports the existence of a relationship between periodontitis and the occurrence of preterm and/or low-birth-weight deliveries. However, the meta-analyses available to date addressing the issue of reversibility (i.e., whether periodontal treatment reduces adverse outcomes of pregnancy) are inconclusive22,23 (Table 2). In any case, it remains important to promote good oral hygiene during routine prenatal visits.
Preeclampsia
Preeclampsia, a condition characterized by high blood pressure and proteinuria during pregnancy after 20 weeks’ gestation, is a major cause of maternal and neonatal mortality and morbidity in the United States and around the world.24 A 2008 systematic review and meta-analysis25 investigated the potential association between periodontitis and several conditions, including maternal infection and preeclampsia. Six studies involving a total of 493 women with preeclampsia and 2927 controls (women without preeclampsia) were pooled for meta-analysis. There was an increased risk of preeclampsia among pregnant women with periodontal disease (pooled OR 1.76, 95% CI 1.43–2.18). In addition, a recent Brazilian case-control study26 showed a similar level of risk (OR 1.52, 95% CI 1.01–2.29). However, another recent case-control study27 showed no clinically meaningful differences between cases and controls with regard to periodontal parameters, regardless of the diagnostic criteria used to define periodontal disease. This area has not been well investigated, and although the data appear to point toward an association between preeclampsia and periodontitis, reversibility has not been demonstrated. Regardless, this finding parallels the data pertaining to preterm and low-birth-weight infants.
Respiratory Diseases
Pneumonia (including community-acquired, hospital-acquired, ventilator-associated and aspiration pneumonia) is an acute condition with gradual onset of cough, with little or no fever.28 Despite adequate treatment, morbidity and mortality rates are high in certain situations (e.g. ventilator-associated pneumonia).29 In the United States, the estimated annual costs of community-acquired pneumonia are as high as $385 million for outpatient care and $8.4 billion for inpatient treatment.30 As well, chronic obstructive pulmonary disease (COPD), characterized by reduced airflow and other breathing-related problems, was the cause of 4% of all deaths in Canada in 2004 (5152 deaths among men and 4455 deaths among women).31 The mortality rate associated with COPD may actually be higher than this, because 2 complications of the condition, pneumonia and congestive heart failure, may be listed as the cause of death for individuals with COPD.31
Our group carried out a systematic review of randomized controlled clinical trials and longitudinal, cohort, case-control and epidemiologic studies (up to 2005), to evaluate a possible link between periodontal disease and respiratory diseases (i.e., COPD or pneumonia).32 There was fairly good evidence for an association between pneumonia and poor oral health (OR 1.2–9.6, depending on oral health indicators used). However, only a weak association (OR < 2.0) was found between COPD and oral health. There was good evidence for reversibility: dental treatment and the establishment of good oral health through topical antimicrobial prophylaxis (polymyxin-neomycin-vancomycin or gentamicin-colistin-vancomycin), decontamination of dental plaque with 0.2% chlorhexidine gel or 0.12% chlorhexidine gluconate oral rinse, and/or professional mouth cleaning (brushing by caregivers and/or mechanical scaling of teeth by dental professionals) led to significant reductions in the occurrence of respiratory diseases among high-risk elderly adults living in nursing homes, especially those in intensive care units (number needed to treat 2–16; relative risk reduction 34%–83%). As such, there is good evidence to support the presence of a significant relationship between respiratory diseases and periodontitis.
Conclusions
The findings reported here are based on the highest levels of evidence currently available in the literature. From these findings, it can be concluded that individuals with periodontitis have a significantly increased probability of greater risk for other problems, including CVD, diabetes, respiratory diseases and preterm delivery of low-birth-weight infants. Many of the research syntheses summarized here were characterized by heterogeneity among studies (e.g., variability in how periodontitis and other diseases were diagnosed). For example, in some studies that were included in the syntheses, diseases were assessed by questionnaire, with no clinical examination. It is also important to realize that patients with certain signs of periodontitis may not have active periodontitis, which could confound the findings of cohort studies, especially interventional trials.
In addition, in some studies, the findings were not necessarily adjusted for participants’ socioeconomic status, which is known to be one of the most profound confounders for almost all disease states. Given these caveats, and until further results from well-designed randomized controlled trials are available, it remains important to recommend periodontal treatment for all patients, whether or not they have other established general health problems, primarily to improve periodontal health in its own right. Despite some evidence for reversibility, it cannot be guaranteed that treatment of periodontitis will reduce patients’ risk for other diseases. However, the role of periodontal disease as a “risk indicator” or “marker” should not be ignored, since the presence of this condition may serve as a warning to the dentist or dental hygienist that the patient is at risk for other diseases, especially CVD, diabetes, respiratory disease and preterm and/or low-birth-weight delivery. Such patients should be informed of the potential for increased risk to allow them to seek appropriate medical investigation or intervention.
THE AUTHORS
References
- US Department of Health and Human Services. Oral health in America: a report of the Surgeon General — Executive summary. Rockville, MD: US Department of Health and Human Services, National Institute of Dental and Craniofacial Research, National Institutes of Health, 2000.
- Fletcher RW, Fletcher SW. Clinical epidemiology: the essentials. 4th ed. Baltimore, MD: Lippincott Williams & Wilkins; 2005.
- Public Health Agency of Canada. Tracking heart disease and stroke in Canada. Ottawa, ON: Public Health Agency of Canada; 2009. Available: www.phac-aspc.gc.ca/publicat/2009/cvd-avc/index-eng.php (accessed 2012 Feb 16).
- Janket SJ, Baird AE, Chuang SK, Jones JA. Meta-analysis of periodontal disease and risk of coronary heart disease and stroke. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003;95(5):559-69.
- Khader YS, Albashaireh ZS, Alomari MA. Periodontal diseases and the risk of coronary heart and cerebrovascular diseases: a meta-analysis. J Periodontol. 2004;75(8):1046-53.
- Bahekar AA, Singh S, Saha S, Molnar J, Arora R. The prevalence and incidence of coronary heart disease is significantly increased in periodontitis: a meta-analysis. Am Heart J. 2007;154(5):830-7. Epub 2007 Aug 20.
- Mustapha IZ, Debrey S, Oladubu M, Ugarte R. Markers of systemic bacterial exposure in periodontal disease and cardiovascular disease risk: a systematic review and meta-analysis. J Periodontol. 2007;78(12):2289-302.
- Humphrey LL, Fu R, Buckley DI, Freeman M, Helfand M. Periodontal disease and coronary heart disease incidence: a systematic review and meta-analysis. J Gen Intern Med. 2008;23(12):2079-86. Epub 2008 Sep 20.
- Blaizot A, Vergnes JN, Nuwwareh S, Amar J, Sixou M. Periodontal diseases and cardiovascular events: meta-analysis of observational studies. Int Dent J. 2009;59(4):197-209.
- Ioannidou E, Malekzadeh T, Dongari-Bagtzoglou A. Effect of periodontal treatment on serum C-reactive protein levels: a systematic review and meta-analysis. J Periodontol. 2006;77(10):1635-42.
- Tonetti MS, D’Aiuto F, Nibali L, Donald A, Storry C, Parkar M, et al. Treatment of periodontitis and endothelial function. N Engl J Med. 2007;356(9):911-20.
- Centers for Disease Control and Prevention. National diabetes fact sheet: national estimates and general information on diabetes and prediabetes in the United States, 2011. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2011.
- Khader YS, Dauod AS, El-Qaderi SS, Alkafajei A, Batayha WQ. Periodontal status of diabetics compared with nondiabetics: a meta-analysis. J Diabetes Complications. 2006;20(1):59-68.
- Simpson TC, Needleman I, Wild SH, Moles DR, Mills EJ. Treatment of periodontal disease for glycaemic control in people with diabetes. Cochrane Database Syst Rev. 2010(5):CD004714.
- Donnelly R, Emslie-Smith AM, Gardner ID, Morris AD. ABC of arterial and venous disease: vascular complications of diabetes. BMJ. 2000;320(7241):1062-6.
- Vergnes JN, Arrive E, Gourdy P, Hanaire H, Rigalleau V, Gin H, et al. Periodontal treatment to improve glycaemic control in diabetic patients: study protocol of the randomized, controlled DIAPERIO trial. Trials. 2009;10:65.
- World Health Organization. International statistical classification of diseases and related health problems. 10th revision. Geneva: World Health Organization; 2011. Available: www.who.int/classifications/icd/ICD10Volume2_en_2010.pdf (accessed 2012 Feb 16).
- Hoyert DL, Mathews TJ, Menacker F, Strobino DM, Guyer B. Annual summary of vital statistics: 2004. Pediatrics. 2006;117(1):168-83.
- Canadian Institute for Health Information. Highlights of 2009–2010 selected indicators describing the birthing process in Canada. Bulletin. May 12, 2011. Available: http://secure.cihi.ca/cihiweb/products/quickstats_childbirth_2009_10_highlight_en.pdf (accessed 2012 Feb 21).
- Vergnes JN, Sixou M. Preterm low birth weight and maternal periodontal status: a meta-analysis. Am J Obstet Gynecol. 2007;196(2):135.e1-7.
- Canadian Institute for Health Information, Too early, too small: a profile of small babies across Canada. Ottawa, ON: CIHI; 2009. Available: http://secure.cihi.ca/cihiweb/products/too_early_too_small_en.pdf (accessed 2012 Feb 21).
- Xiong X, Buekens P, Vastardis S, Yu SM. Periodontal disease and pregnancy outcomes: state-of-the-science. Obstet Gynecol Surv. 2007;62(9):605-15.
- Polyzos NP, Polyzos IP, Zavos A, Valachis A, Mauri D, Papanikolaou EG, et al. Obstetric outcomes after treatment of periodontal disease during pregnancy: systematic review and meta-analysis. BMJ. 2010;341:c7017.
- Roberts JM, Pearson G, Cutler J, Lindheimer M; NHLBI Working Group on Research on Hypertension During Pregnancy. Summary of the NHLBI Working Group on Research on Hypertension During Pregnancy. Hypertension. 2003;41(3):437-45.
- Conde-Agudelo A, Villar J, Lindheimer M. Maternal infection and risk of preeclampsia: systematic review and metaanalysis. Am J Obstet Gynecol. 2008;198(1):7-22.
- Siqueira FM, Cota LO, Costa JE, Haddad JP, Lana AM, Costa FO. Maternal periodontitis as a potential risk variable for preeclampsia: a case-control study. J Periodontol. 2008;79(2):207-15.
- Lohsoonthorn V, Kungsadalpipob K, Chanchareonsook P, Limpongsanurak S, Vanichjakvong O, Sutdhibhisal S, et al. Maternal periodontal disease and risk of preeclampsia: a case-control study. Am J Hypertens. 2009;22(4):457-63. Epub 2009 Jan 22.
- Centers for Disease Control and Prevention. Chlamydia pneumoniae. Atlanta, GA: National Center for Immunization and Respiratory Diseases: Division of Bacterial Diseases; 2005. Available: www.cdc.gov/ncidod/dbmd/diseaseinfo/chlamydiapneumonia_t.htm (accessed 2012 Feb 16).
- Pugin J, Auckenthaler R, Lew DP, Suter PM. Oropharyngeal decontamination decreases incidence of ventilator-associated pneumonia. A randomized, placebo-controlled, double-blind clinical trial. JAMA. 1991;265(20):2704-10.
- Amin AN, Feinbloom D, Krekun S, Li J, Pak M, Rauch DA, et al. Recommendations for management of community- and hospital-acquired pneumonia -- the hospitalist perspective. Curr Opin Pulm Med. 2004;10 Suppl 1:S23-7.
- Public Health Agency of Canada. Life and breath: respiratory disease in Canada, 2007. Ottawa, ON: Public Health Agency of Canada; 2007. Available: www.phac-aspc.gc.ca/publicat/2007/lbrdc-vsmrc/pdf/PHAC-Respiratory-WEB-eng.pdf (accessed 2012 Feb 16).
- Azarpazhooh A, Leake JL. Systematic review of the association between respiratory diseases and oral health. J Periodontol. 2006;77(9):1465-82.
